What causes multiple sclerosis remains one of the most asked questions in neurology today. Multiple sclerosis, or MS, affects millions of people worldwide, yet scientists still cannot point to one single cause. The condition develops when your immune system attacks the protective covering of nerves, which disrupts communication between your brain and body.
Research has identified several factors that may contribute to MS, including genetics, immune system problems, infections, and environmental triggers. Each person’s experience with MS is different, and the combination of risk factors varies from one individual to another. This guide explores what current research tells us about MS causes in 2026.
What Is Multiple Sclerosis?
Multiple sclerosis is a chronic disease that affects the central nervous system. Your brain and spinal cord make up this system, and MS causes inflammation and damage to nerve fibers.
Basic Overview of Multiple Sclerosis
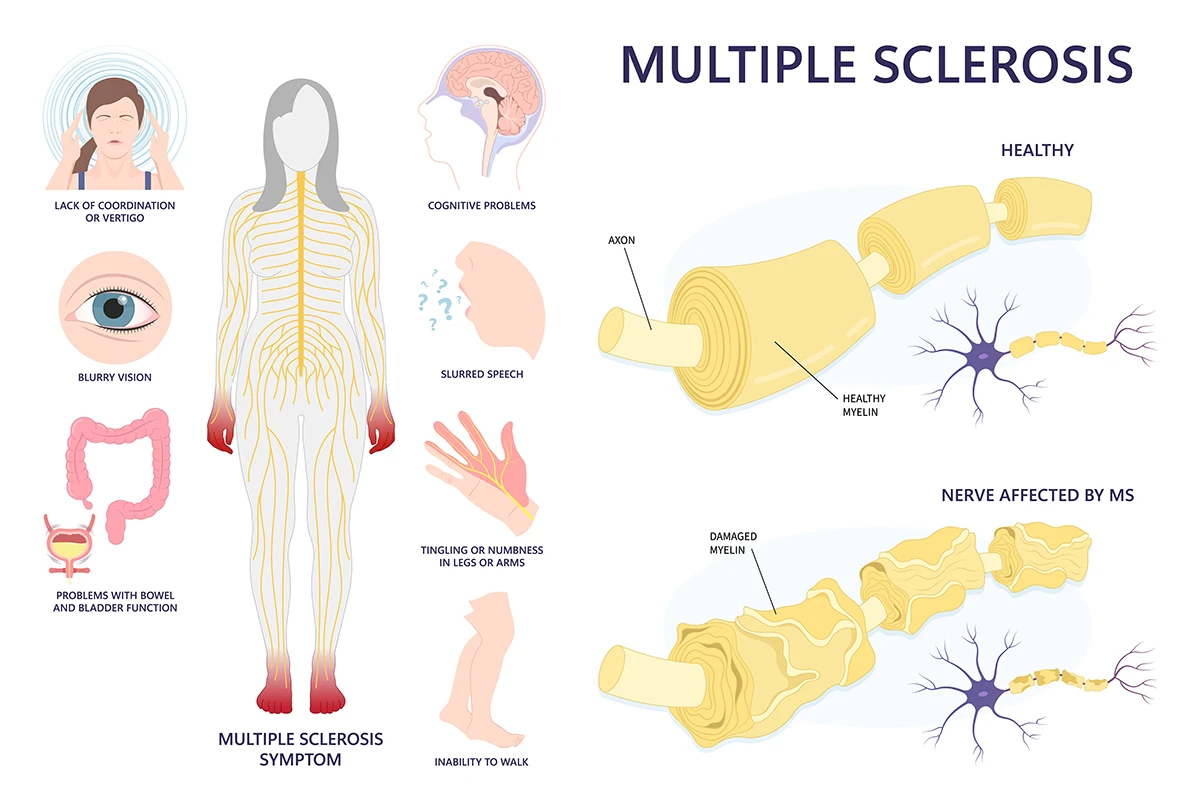
MS happens when your immune system mistakenly attacks healthy neural tissue. It specifically targets myelin, which is the protective coating around nerve fibers. When this coating gets damaged, nerve signals slow down or stop completely.
Scar tissue forms in place of damaged myelin. These scars are called lesions or plaques. The disease gets its name from the multiple areas of scarring throughout the nervous system.
Common symptoms include vision problems, numbness, weakness, and balance issues. Some people experience fatigue, pain, or cognitive changes. The severity and progression differ greatly among individuals.
How Does MS Develop in the Nervous System?
MS development starts with immune system dysfunction. Certain immune cells mistakenly enter rthe brain and spinal cord. Normally, these areas are protected by a barrier that keeps most immune cells out. In MS, this protective barrier becomes ‘leaky’ and allows immune cells to pass through.
Once inside, these cells wrongly identify myelin as something harmful and start attacking it, inflammation and damage. As myelin breaks down, nerve impulses cannot travel properly between your brain and body, disrupting normal nerve function.
Over time, the nerves themselves can become damaged too. This can lead to lasting symptoms and, in some cases, permanent disability. For some people, the disease occurs in flare ups followed by periods of recovery. For others, it gradually worsens over time.
Is There a Single Cause of Multiple Sclerosis?
No single factor causes MS on its own. Research shows that multiple elements must come together to trigger the disease. Scientists have studied this condition for decades and found many pieces contribute to the puzzle.
Why Doesn't MS Have One Exact Cause?
The complexity of MS stems from how different body systems interact with each other. Your genes provide one layer of influence that determines your baseline risk. Your environment adds another layer through exposures to sunlight, viruses, and lifestyle factors.
Two people with similar genetics might not both develop MS. This shows that genetics alone cannot explain the disease. Likewise, exposure to certain risk factors does not automatically lead to MS.
Here’s what we know about why MS doesn’t have a single cause:
- Each risk factor contributes a small piece to overall disease development
- Genetic susceptibility sets the stage but doesn't guarantee you'll get MS
- Environmental exposures act as triggers only in some individuals
- Timing of exposures during your life makes a significant difference
- Your unique combination of factors determines whether you develop MS
How Do Multiple Factors Work Together?
Think of MS risk like a combination lock. You need several numbers in the right sequence to open it. Scientists call this the “multiple hit hypothesis” because each risk factor is considered a separate ‘hit’ that can contribute to its development.
MS risk appears to develop from a combination of factors working together over time:
- Genetics might make you susceptible to immune system problems
- An infection could activate your immune system incorrectly
- Low vitamin D might weaken your body's defenses against inflammation
- Stress could add another burden to an already challenged system
Role of the Immune System in Multiple Sclerosis
How Does Autoimmune Response Trigger MS?
The autoimmune process in MS follows a specific pattern. A trigger causes your immune system to become overactive, causing certain immune cells to become activated and start behaving abnormally.
These immune cells then cross that protective barrier and enter your central nervous system. Once inside, they recruit other immune cells to join the attack. This creates a cycle of inflammation and damage that feeds on itself.
Here’s what happens during an autoimmune attack in MS:
- Your T cells mistakenly identify myelin proteins as foreign invaders
- These activated cells cross into your brain and spinal cord
- They signal other immune cells to join the attack
- B cells produce antibodies that target and damage myelin coating
- Inflammation causes swelling and disrupts normal nerve function
- Each wave of attack creates new damage and scar tissue
Why Does the Immune System Attack Myelin?
Scientists have several theories about this misdirected immune response. One theory involves molecular mimicry, which happens when a virus mimics proteins similar to myelin proteins. Instead of attacking the virus, your immune system gets confused and attacks myelin too.
Another theory focuses on genetic mutations that affect immune regulation. Some people have genes that make their immune cells more aggressive than normal. A third possibility involves a breakdown in immune tolerance, where your body fails to train immune cells properly.
Genetic Factors Linked to Multiple Sclerosis
Genetics contributes significantly to MS risk in complex ways. Research has identified over 200 genetic variants associated with MS, though each variant has only a small effect on its own.
Does MS Run in Families?
MS does show some family clustering. If one parent has MS, your lifetime risk is about 2 to 3 percent. This is higher than the general population risk of around 0.1 percent.
Studies show that if one identical twin has MS, the other twin develops it only about 25 to 30 percent of the time. That also means that in 70 to 75 percent of identical twin pairs, the second twin does not develop MS. Since identical twins share the same DNA, this shows that genetics alone cannot fully explain why MS develops.
Researchers have identified certain genes that appear more often in people with MS. These genes are mostly linked to how the immune system works. One of the strongest links is a gene called HLA-DRB1. It plays a role in helping your immune system tell the difference between your body’s own cells and foreign substances. Some versions of this gene are associated with a higher risk of developing MS.
Other genes that may play a role include:
- Variations of the HLA-DRB1 gene, which are linked to a higher risk
- The IL2RA gene, which helps regulate how immune cells communicate
- The IL7R gene, which is involved in the development and activity of certain immune cells
- Genes related to the vitamin D receptor, which affect how the body responds to vitamin D
- Many other genetic variations that each contribute a small amount to overall risk
No single gene causes MS on its own. Instead, risk appears to result from the combined effect of many small genetic differences working together.
Why Don't Genetics Alone Cause MS?
Even though identical twins share the same DNA, it is common for one twin to develop the condition while the other does not. This suggests that environmental factors and life experiences also play an important role. Most genetic variants found in MS studies are common in the population. Many people carry these variants without ever developing MS.
The genes create susceptibility rather than certainty. Environmental triggers seem necessary to activate the genetic risk. This explains why MS rates vary by geographic location.

Environmental Factors That May Trigger MS
Where you live and what you are exposed to affects your MS risk. Several environmental factors have strong research support backing their connection to MS.
Low Vitamin D and Sunlight Exposure
Vitamin D deficiency has emerged as a major environmental risk factor for MS. People with low vitamin D levels consistently show higher MS rates. Sunlight helps your skin produce vitamin D naturally.
Studies show that higher vitamin D levels may protect against MS. People born in autumn have slightly higher MS risk because they had less sun exposure during pregnancy. Vitamin D helps regulate your immune system by keeping immune responses balanced.
Geographic Location and MS Risk
MS rates increase steadily the farther you get from the equator. Countries near the equator have very low MS rates. Places like Canada, Scotland, and Norway have some of the highest rates.
Migration studies provide valuable insights. People who move from high-risk to low-risk areas before puberty adopt the lower risk. Those who move after puberty keep their original risk level. This points to childhood as a critical period.
Childhood Environment and Early Life Exposure
Your early environment appears to play an important role in shaping future MS risk. Research suggests that being raised in rural settings is linked to a slightly lower likelihood of developing MS. One possible reason is increased exposure to everyday microbes during childhood.
Growing up around farm animals, spending time outdoors, or having several siblings can increase contact with common viruses, bacteria, soil, and other natural elements. These routine exposures may help train the developing immune system to respond appropriately to threats.
This idea aligns with what researchers call the hygiene hypothesis. It suggests that when the immune system encounters a variety of normal environmental challenges early in life, it learns balance. Without enough of these exposures during key developmental periods, the immune system may be more likely to respond inappropriately later on.
Viral and Infectious Triggers
Infections, especially viral ones, are strongly linked to what causes multiple sclerosis. Recent research has focused heavily on one virus in particular.
Connection Between Epstein Barr Virus and MS
Epstein Barr Virus (EBV) has the strongest link to MS. Nearly 100 percent of people with MS have been infected with EBV. A major 2022 study tracked over 10 million military personnel. It found that EBV infection increased MS risk by 32 times.
But EBV alone does not cause MS. Billions of people have EBV without getting MS. The virus might trigger MS only in genetically susceptible people. Scientists think EBV could activate the immune system incorrectly in vulnerable individuals.
How Do Past Infections Affect MS Risk?
Beyond EBV, other infections have been studied as potential triggers. Some research suggests that multiple childhood infections might increase risk. However, the hygiene hypothesis suggests early exposure to common germs might protect you.
Timing seems crucial. Some infections might be protected if they occur early in life. The same infections might increase risk if they occur during adolescence.
Your Condition May Qualify for Alternative Treatment
Lifestyle Factors That May Increase MS Risk
Your daily habits and lifestyle choices influence MS risk in measurable ways. Research has identified several lifestyle behaviors consistently associated with higher MS rates.
Smoking and its Link to MS
Smoking is associated with an increased risk of developing MS. Research suggests that current smokers have a higher risk compared to people who have never smoked. Smoking has also been linked to faster disease progression in individuals who already have MS.
Cigarette smoke promotes inflammation throughout the body and affects immune system function. Some studies suggest it may influence the integrity of the blood–brain barrier, the protective layer around the brain and spinal cord, potentially allowing more immune activity in the central nervous system. However, MS development is complex, and smoking is considered one contributing factor rather than a direct cause.
The good news is that quitting smoking is associated with a gradual reduction in risk over time.
Obesity and MS Risk
Being overweight or obese as you develop significantly increases your future MS risk. Studies show that teenage obesity roughly doubles the risk of developing MS later. Excess body fat produces inflammatory chemicals that keep your immune system activated.
Obesity also affects vitamin D levels. Fat tissue can trap vitamin D, making it less available for immune regulation. Maintaining a healthy weight during youth could help protect you.
Stress and Its Possible Role
The relationship between stress and MS is less clear than other lifestyle factors. Some studies suggest chronic stress may be linked to increased risk, but the evidence is still evolving.
Stress can influence the immune system in several ways. Long-term stress may increase inflammation, alter the balance of immune cells, and affect the release of stress hormones like cortisol, which helps regulate immune responses. When these systems are repeatedly disrupted, immune function may become less stable over time.
However, stress alone is not considered a direct cause of MS. It is viewed as one possible contributing factor among many.
Current evidence suggests stress alone probably does not directly cause MS. But it might act as one contributing factor among many. Managing stress effectively has benefits regardless of your MS risk level.
Hormonal and Gender Related Factors
MS affects women substantially more often than men across all populations studied. Understanding what causes multiple sclerosis in females helps explain this persistent gender gap.
Why Is MS More Common in Women?
Women are about three times more likely to develop MS compared to men. This gender ratio has increased over the past several decades. Women generally have more robust immune systems than men do.
This enhanced immunity helps them fight infections more effectively. But it might also make them more vulnerable to autoimmune diseases. The X chromosome contains many genes related to immune system function.
Role of Hormonal Changes in MS Development
Estrogen and other female hormones seem to influence MS risk and disease activity. The disease typically develops during reproductive years when hormone levels fluctuate dramatically. Pregnancy provides fascinating clues about how hormones affect MS.
Here’s what data tells us about hormones and MS:
- Estrogen and progesterone reach very high levels during late pregnancy
- MS relapse rates drop significantly during the third trimester of pregnancy
- These hormones might have protective anti-inflammatory effects on immunity
- After delivery, hormone levels crash dramatically within days
- Relapse rates spike in the first few months after giving birth
Age and Timing of MS Onset
MS typically begins at fairly specific ages. Understanding when symptoms usually start provides valuable clues about underlying disease causes.
When Do MS Symptoms Usually Begin?
Here are key facts about when MS typically begins:
- Peak onset occurs between ages 20 and 40 across most populations
- Average diagnosis age is approximately 30 years old
- The immune system reaches complete maturity during these years
- Hormonal changes continue actively through the twenties
- All these biological factors might combine during this vulnerable period
Why Is Early Adulthood a Common Onset Period?
Childhood is considered an important window for shaping long-term MS risk, as early environmental exposures help lay the foundation for immune system development.
Adolescence and early adulthood, however, are the periods when MS most commonly becomes clinically apparent in people who are already susceptible.
During young adulthood, stress levels often increase due to education, career demands, and major life transitions. Epstein–Barr virus (EBV) infection also frequently occurs during adolescence. In individuals with genetic susceptibility and earlier environmental influences, these additional factors may contribute to the timing of symptom onset.
Can Multiple Risk Factors Lead to MS Together?
Research increasingly shows that what causes multiple sclerosis involves combined and interacting risks. Instead, multiple hits accumulate over many years to trigger MS development.
How Do Genetics and Environment Interact?
Gene-environment interactions are key to understanding MS causes fully. Your genes set your baseline risk level. Environmental factors can then substantially increase or decrease that inherited risk.
Here’s how genes and environment work together:
- Certain gene variants change how your body processes vitamin D
- People with these variants might be more sensitive to vitamin D deficiency
- Some genes affect immune responses to infections like EBV
- People with these variants might react more strongly to viral infections
- Smoking might also interact with specific genetic variants
- The harmful effects could be worse in genetically susceptible people
Why Do Risk Factors Differ from Person to Person?
Everyone has a completely unique combination of risk factors. Two people with MS might have totally different risk profiles. One person might have strong genetic risk, but few environmental triggers.
Scientists are working to develop personalized risk assessments. For now, reducing all modifiable risk factors makes sense for everyone. Even if you have genetic risk, reducing environmental triggers helps protect you.
Can MS Be Prevented If the Causes Are Known?
Knowing risk factors does not guarantee prevention of MS. MS is too complex for simple prevention strategies. However, understanding probable causes can help reduce your personal risk substantially.
What Can and Cannot Be Controlled?
You cannot change your genetic inheritance or family history. Your childhood environment and past infections are already determined. But many important risk factors remain within your control.
You can control vitamin D levels through supplementation and sun exposure. Smoking cessation is entirely within your power. Maintaining a healthy weight through diet and exercise is achievable. Managing stress effectively requires effort but is possible.
Steps That May Help Lower Risk
Several practical steps can potentially reduce your MS risk. Here’s what you can do to lower your chances.
- Maintain adequate vitamin D levels through supplements or safe sun exposure. Most experts recommend 1000 to 2000 IU daily. Get your blood levels checked regularly.
- Avoid smoking completely and minimize secondhand smoke exposure. If you currently smoke, quitting provides benefits at any age. Your risk decreases the longer you stay smoke-free.
- Stay physically active and maintain a healthy weight consistently. Regular exercise supports immune function and reduces inflammation. Focus especially on maintaining healthy weight during adolescence.
- Manage infections appropriately, especially during childhood. Practice good hygiene and stay current with recommended vaccinations. Treat infections promptly when they occur.
- Reduce chronic stress through healthy coping strategies. Exercise, sleep, social support, and relaxation techniques all help. Find stress management methods that work for you.
- Consider your family history when making health decisions. If you have relatives with MS, be extra vigilant about modifiable risks.
When to Talk to a Healthcare Professional?
Early detection and treatment of MS can dramatically improve long-term outcomes. Several specific warning signs should prompt a visit to your doctor.
Early Symptoms That Should Not Be Ignored
MS symptoms vary widely but some common patterns exist. Here are symptoms that warrant medical attention.
- Vision changes like blurred vision, double vision, or eye pain. Sudden vision loss requires immediate attention.
- Numbness or tingling in your limbs that comes and goes. It can affect arms, legs, or face.
- Weakness in your arms or legs that develops gradually. Difficulty walking or maintaining balance.
- Profound fatigue that interferes with daily activities. This is not normal tiredness but exhaustion.
- Dizziness or vertigo with balance problems.
- Bladder or bowel control issues.
- Cognitive changes like memory problems or difficulty concentrating.
Importance of Early Evaluation
Getting evaluated early helps in several ways. Many conditions besides MS can cause similar symptoms. These need to be ruled out through proper testing.
Here’s why early evaluation is important:
- Proper testing can rule out other conditions with similar symptoms
- If you do have MS, early treatment works much better
- Disease-modifying therapies can slow progression significantly
- Starting treatments early preserves more function over time
- Early diagnosis helps you plan and make informed decisions
- Knowledge allows you to take control of your situation
Early evaluation typically includes a neurological exam. Your doctor will test your reflexes, coordination, and sensation. They might order MRI scans to look for brain or spinal cord lesions.
Final Thoughts
What causes multiple sclerosis remains incompletely understood in 2026. But research has revealed many important pieces of this complex puzzle. MS develops when multiple factors combine in genetically susceptible individuals.
Genetics provides the foundation for risk. Environmental triggers like low vitamin D and infections add to that risk. Lifestyle choices such as smoking and obesity contribute as well. Hormonal factors explain why women are more affected.
Your specific combination of risk factors determines your individual journey. While MS cannot be prevented with certainty, you can reduce modifiable risks. Maintaining vitamin D levels, avoiding smoking, and staying healthy and physically fit all help substantially.
Understanding possible causes empowers you to make informed choices. It also helps you recognize when to seek medical evaluation. Early detection and treatment improve outcomes significantly.
Continue following research developments as science advances. New discoveries about MS causes emerge regularly. Stay informed, maintain your health, and work closely with healthcare providers.
Frequently Asked Question
What is the main cause of multiple sclerosis?
Is multiple sclerosis caused by genetics or environment?
Can stress cause multiple sclerosis?
Does vitamin D deficiency increase MS risk?
Can infections trigger multiple sclerosis?
Certain infections, especially Epstein Barr Virus (EBV), are strongly linked to MS. Nearly all people with MS have been infected with EBV. Research shows EBV infection increases MS risk by up to 32 times. However, billions of people have EBV without developing MS. The virus likely triggers disease only in genetically susceptible individuals.