Introduction
Primary progressive multiple sclerosis (PPMS) is one of the main types of Multiple Sclerosis (MS) that affects people differently. If you or someone you care about has MS, understanding the different types helps you know what to expect. MS comes in several forms, and two progressive types often confuse people.
PPMS and secondary progressive MS (SPMS) both involve gradual worsening. But they develop in completely different ways. One starts with steady decline from the beginning. The other develops after years of relapses and remissions.
Knowing the difference helps you understand your diagnosis better. It also helps you have more informed conversations with your healthcare team. This guide breaks down the key differences in simple terms.
What Is the Main Difference Between PPMS and SPMS?
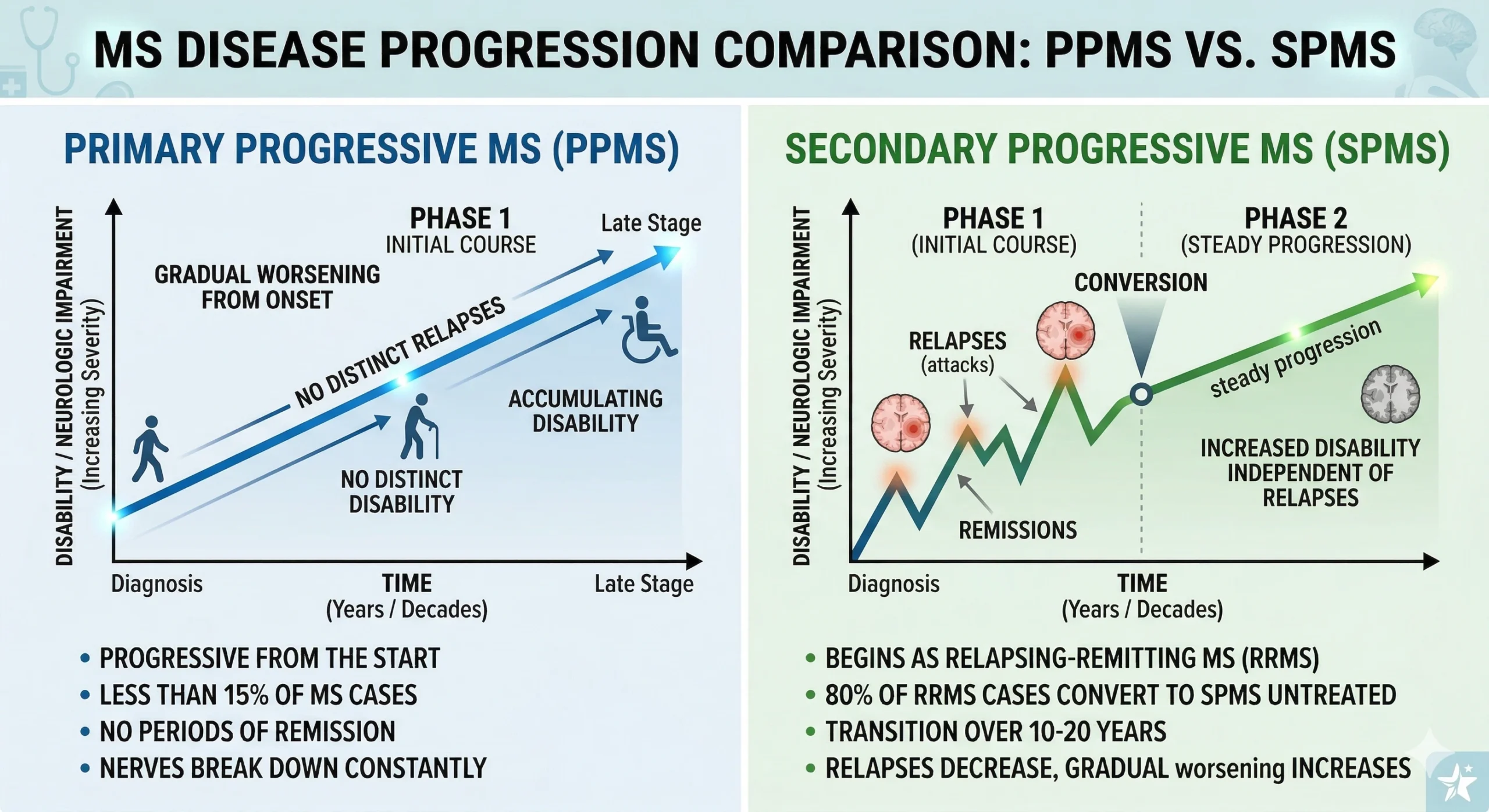
The biggest difference between these two types lies in how they start. PPMS begins with gradual worsening from day one. SPMS develops after someone has had relapsing remitting MS for years.
This fundamental difference affects everything about how the disease behaves. It influences symptoms, progression patterns, and even treatment options. Understanding this distinction helps you recognize which type you might be dealing with.
| Feature | Primary Progressive MS (PPMS) | Secondary Progressive MS (SPMS) |
|---|---|---|
| Initial Pattern | Steady progression from onset | Starts as relapsing remitting MS |
| Early Relapses | No distinct relapses | Clear relapses and remissions |
| Disease History | Progressive from day one | Years of RRMS (relapsing-remitting multiple sclerosis) before progression |
| Progression Pattern | Continuous gradual decline | Transition from relapses to steady decline |
| Typical Age at Onset | Around 40 years or older | Usually 40-50 years (transition age) |
| Gender Distribution | Equal in men and women | More common in women |
| Prevalence | 10-15% of all MS cases | About 50% of RRMS cases transition |
Does One Start with Relapses While the Other Does Not?
Yes, and this is the clearest way to tell them apart. PPMS never has distinct relapses at the beginning. Symptoms gradually worsen from the very start without clear attacks or recovery periods.
SPMS is completely different. It always starts as relapsing remitting MS first. People experience clear attacks followed by partial or complete recovery. After several years, the pattern changes and symptoms start worsening steadily.
This history of relapses is what separates the two types. If you had relapses early on, you have SPMS. If you never had relapses and symptoms just got worse steadily, you have PPMS.
How Does Symptom Worsening Look Different in Each Type?
The progression patterns show distinct differences between these two types of MS. Understanding these patterns helps you recognize what to expect.
In PPMS, the worsening follows a predictable path:
- Symptoms gradually accumulate from the very beginning without fluctuation
- Imagine a car travelling on a ramp going slowly but consistently downhill over time
- There are no clear periods of improvement or stability early on
- Each month brings subtle but measurable decline in function
- The steady nature makes it easier to track progression over time
SPMS shows a completely different pattern:
- It starts with ups and downs from relapses and recovery periods
- You experience years of attacks followed by partial or complete remissions
- Then the pattern shifts to steady decline after the transition
- You might still have some relapses on top of the steady worsening
- The progression can be harder to identify because of ongoing fluctuations
The progression rate can vary in both types. Some people progress slowly while others decline faster. But the overall pattern remains distinct between the two types.
What Is Primary Progressive Multiple Sclerosis?
PPMS accounts for about 10 to 15 percent of all MS cases. It develops differently than other MS types and often affects people at a different ages.
This type involves steady neurological decline from the very beginning. There are no clear relapses or remissions. Symptoms simply accumulate and worsen over time.
How Does PPMS Begin?
PPMS typically starts quietly without the dramatic symptoms seen in other types. The gradual onset makes it challenging to identify early on.
Here’s how primary progressive MS usually develops:
- You might notice subtle changes in walking or balance first
- These changes gradually worsen over months and years
- Unlike relapsing remitting MS, there is no sudden onset of symptoms
- You will not wake up one day with vision loss or severe numbness
- Instead, symptoms creep in slowly and persistently over time
- Many people do not realize something is wrong at first
- The gradual nature makes it easy to dismiss early symptoms as aging
- By the time you seek help, progression has usually been happening for a while
Do Symptoms Get Worse Slowly Over Time?
Yes, steady worsening defines PPMS. Symptoms accumulate gradually without periods of improvement. Each month or year brings subtle but measurable decline.
Walking problems are often the most noticeable symptom. You might need a cane first, then a walker, then eventually a wheelchair. The timeline varies greatly from person to person.
Other symptoms also progress steadily. These include bladder problems, muscle stiffness, and cognitive changes. The rate of progression differs among individuals.
Who Is More Likely to Develop PPMS?
Primary progressive MS affects certain groups of people more commonly. Understanding these patterns helps identify who might be at higher risk.
Key characteristics of people who develop PPMS include:
- The disease typically starts later in life, usually around age 40 or older
- This is about 10 years later than relapsing remitting MS typically begins
- Men and women develop PPMS at roughly equal rates
- This differs from relapsing remitting MS, which affects far more women
- The equal gender distribution is unique to this type of MS
- People with PPMS often experience more spinal cord involvement early on
- This explains why walking problems are so common from the beginning
- Brain lesions tend to be less prominent compared to other MS types
What Is Secondary Progressive Multiple Sclerosis?
SPMS develops after years of relapsing remitting MS. About 50 percent of people with RRMS eventually transition to this type. This usually happens within 10 to 20 years of initial diagnosis.
The transition marks a significant change in disease behavior. Instead of distinct attacks and recoveries, symptoms start worsening steadily. This shift often happens gradually and can be hard to identify.
How Does SPMS Develop After RRMS?
The transition from RRMS to secondary progressive multiple sclerosis happens slowly and often goes unnoticed at first. Understanding the progression helps you identify when the shift occurs.
Here’s how the transition typically unfolds:
- Your relapses might become less frequent over time
- Recovery from relapses becomes increasingly incomplete
- You notice you don't bounce back to your previous baseline anymore
- Disability starts accumulating between relapses instead of just during them
- Baseline function worsens even without obvious attacks or new symptoms
- Walking becomes progressively harder regardless of relapse activity
- Fatigue increases steadily over months and years
- Cognitive problems grow more persistent between attacks
- These changes happen independently of clear relapses
The shift can take months or years to become obvious. Many people look back and realize they have been in SPMS for a while. Doctors often confirm the transition retrospectively.
When Does Relapsing Remitting MS Turn Into SPMS?
The timing varies significantly from person to person. Some people transition within 5 to 10 years of diagnosis. Others remain in RRMS for 20 years or more before shifting.
Several factors influence when transition happens. Earlier age at RRMS onset often means longer time before SPMS. More frequent early relapses might lead to faster transition. Incomplete recovery from relapses can signal coming progression.
The multiple sclerosis secondary progressive stage often starts between ages 40 and 50. But this timeline is not fixed. Some people never transition to SPMS at all.
Do Relapses Stop in SPMS?
Relapses do not always stop completely in secondary progressive MS. Many people continue having occasional attacks on top of steady progression. These relapses might become less frequent over time.
Some people transition to SPMS without relapses at all. Their disease simply shifts to steady worsening without any attacks. This makes distinguishing SPMS from PPMS more challenging.
The key difference is the pattern of worsening. In SPMS, disability accumulates steadily regardless of relapses. In RRMS, disability mainly occurs during and after attacks.
How Do Symptoms Compare Between PPMS and SPMS?
Both progressive types share many common symptoms. Walking difficulties, muscle stiffness, bladder problems, and fatigue affect both groups. However, the pattern and timing of symptoms differ.
The symptoms themselves overlap significantly. But how they develop and progress shows clear differences. Understanding these patterns helps distinguish between the two types.
Is Walking Difficulty More Common in One Type?
Walking problems are especially prominent in primary progressive MS. This symptom often appears first and progresses steadily. Many people with PPMS need mobility aids earlier than other MS types.
Secondary progressive MS also causes walking difficulties. But these often develop after other symptoms have appeared. The progression might be more variable depending on relapse patterns.
Both types eventually lead to significant mobility challenges. The timeline and pattern just differ. PPMS shows steady decline while SPMS might have periods of stability mixed with worsening.
Do Both Types Affect Vision and Balance?
Yes, both types can affect vision and balance. But the patterns differ based on disease history. Vision problems are more common in early RRMS before transition to SPMS.
Balance issues affect both types significantly. In PPMS, balance problems often develop gradually alongside walking difficulties. In SPMS, balance might worsen during relapses or as part of steady progression.
Dizziness and vertigo can occur in both types. The severity and persistence vary among individuals. Some people experience constant balance problems while others have intermittent issues.
Does Fatigue Feel Different in PPMS vs SPMS?
Fatigue is overwhelming in both progressive types. The exhaustion goes beyond normal tiredness. It can make daily activities extremely challenging.
The pattern of fatigue might differ slightly. PPMS fatigue tends to be constant and gradually worsening. SPMS fatigue might fluctuate more, especially if relapses continue.
Both types can cause physical and cognitive fatigue. Your body feels exhausted even after rest. Your mind feels foggy and thinking requires extra effort.
Can Secondary Progressive MS Look Like Primary Progressive MS?
Sometimes secondary progressive MS can closely resemble primary progressive MS. This happens when someone transitions to SPMS without continuing relapses. The steady progression looks similar in both types.
However, the disease history always reveals the difference. Looking back at how symptoms started separates the two types clearly.
Why Some Symptoms Overlap
Both progressive types involve chronic inflammation and nerve damage. This shared mechanism explains why symptoms overlap so much. The immune system continues attacking myelin in both cases.
Brain and spinal cord lesions accumulate over time in both types. Nerve damage causes similar problems regardless of disease type. Walking difficulties, cognitive changes, and fatigue result from this damage.
The location of lesions matters more than the MS type sometimes. Spinal cord lesions cause walking problems in both PPMS and SPMS. Brain lesions affect thinking and coordination similarly.
Why Tracking Relapses Is Important
Accurate disease history helps doctors make the right diagnosis. Knowing whether you had early relapses determines your MS type. This information affects treatment decisions and prognosis discussions.
Some people forget about mild early relapses. They might have dismissed temporary numbness or vision changes years ago. Reviewing medical records helps identify these forgotten episodes.
The primary progressive multiple sclerosis diagnosis depends on ruling out previous relapses. Doctors look for evidence of attacks in your history. Without any relapse history, PPMS becomes the likely diagnosis.
Does Treatment Differ Between PPMS and SPMS?
Treatment options do differ somewhat between these two progressive types. Fewer medications are specifically approved for PPMS compared to other MS types. SPMS has more treatment options available.
However, both types benefit from symptom management and supportive care. Treatments focus on maintaining function and quality of life. The approach depends on individual symptoms and needs.
Are There Approved Medicines for PPMS?
Treatment options for primary progressive MS are more limited than other types. However, recent advances have brought new hope for people with this condition.
Here’s what you need to know about PPMS treatments:
- Treatment options for primary progressive multiple sclerosis (PPMS) are more limited compared to other forms of MS, though research advances have expanded available approaches in recent years.
- There is currently one FDA-approved disease-modifying therapy indicated specifically for PPMS. It targets certain immune cells believed to play a role in myelin damage.
- This therapy may be considered for individuals who show signs of active inflammation on MRI, such as new or enhancing lesions. Eligibility depends on a full clinical evaluation.
- Factors such as age, overall health, and level of disease activity are typically reviewed when assessing suitability. Some evidence suggests earlier use may be associated with better outcomes, though responses vary.
- Not everyone is a candidate, and individual results differ. Treatment decisions are made in consultation with a qualified healthcare provider.
- In addition to disease-modifying therapy, symptom management, rehabilitation strategies, and supportive care remain important components of overall PPMS management.
What Treatments Help in SPMS?
Several therapies are approved for secondary progressive MS (SPMS), particularly in cases where relapses or active inflammation are still present. These treatments are designed to reduce relapse activity and help slow further progression.
Selecting the right approach depends on individual factors. Evidence of active inflammation on MRI, relapse history, and the rate of progression are all considered when evaluating options.
Symptom management also plays an important role in SPMS care. Rehabilitation strategies, including physical therapy, can support mobility and strength. Additional supportive treatments may be used to address specific challenges such as muscle stiffness, discomfort, or bladder concerns, depending on individual needs.
Do Lifestyle Changes Support Both Types?
Healthy lifestyle choices benefit both progressive types significantly. These modifications can improve your quality of life and potentially slow progression.
Here are key lifestyle changes that support both PPMS and SPMS:
- Regular exercise helps maintain mobility and reduces fatigue in both types. Even gentle movement like chair exercises or water aerobics makes a difference. Work with a physical therapist to develop a safe exercise plan.
- A balanced diet supports overall health and immune function effectively. Some people find anti-inflammatory diets helpful for managing symptoms. Focus on whole foods, fruits, vegetables, and lean proteins.
- Staying well-hydrated is especially important for bladder and bowel function. Proper hydration helps prevent urinary tract infections common in progressive MS. Aim for adequate water intake throughout the day.
- Stress management techniques help reduce symptom flares in both types. Chronic stress can worsen MS symptoms and overall wellbeing. Meditation, yoga, or counseling provide valuable support.
- Quality sleep is essential for managing fatigue and cognitive function. Establish a regular sleep schedule and create a restful environment. Address sleep disorders promptly with your healthcare team.
- Avoiding smoking is crucial as it can worsen MS progression. If you smoke, quitting provides significant benefits at any stage. Your healthcare team can help with cessation programs.
Which Type Is More Severe?
Neither type is automatically more severe than the other. Both progressive forms lead to increasing disability over time. Individual experiences vary widely within each type.
Severity depends on multiple factors beyond just MS type. Progression rate, age at onset, and treatment response all matter. Each person’s journey is unique.
Does Faster Progression Mean More Disability?
Generally yes, faster progression leads to more rapid disability accumulation. But progression rate varies significantly among individuals. Some people with PPMS progress very slowly over decades.
Others with SPMS might progress quickly after transition. The rate cannot be predicted with certainty. Regular monitoring helps track changes over time.
MS secondary progressive life expectancy is not dramatically different from other types. MS itself rarely directly causes death. Complications from disability pose the main risks.
Why Severity Is Different for Each Person
Your unique biology affects how MS progresses. Genetic factors influence disease behavior. Environmental factors and lifestyle choices matter too.
Age at onset affects long-term outcomes. Younger onset often allows more years of stability. Older onset might involve faster progression.
Treatment response varies among individuals. Some people respond well to available therapies. Others see less benefit from the same medications.
Can MS Change from One Type to Another?
MS types can change, but only in specific directions. The transition patterns follow predictable paths. Understanding these patterns helps you know what to expect.
Why PPMS Does Not Turn Into SPMS
Primary progressive MS never transitions to secondary progressive MS. This is because SPMS requires a history of relapsing remitting MS first. PPMS starts with progression from day one.
The definitions of these types prevent this transition. PPMS is defined by lack of early relapses. SPMS is defined by progression after initial relapses.
If you start with PPMS, you stay classified as PPMS. The progression pattern might change slightly over time. But the fundamental diagnosis remains the same.
How RRMS Transitions Into SPMS
Relapsing remitting MS commonly transitions to secondary progressive MS over time. This shift happens when steady worsening begins. Disability accumulates between relapses instead of just during them.
The transition is often gradual and hard to pinpoint. Doctors look for sustained worsening over 6 to 12 months, this worsening happens independently of relapses.
Not everyone with RRMS transitions to SPMS. Modern treatments might be changing these patterns. Some people remain in RRMS for their entire lives.
Final Thoughts
Primary progressive MS and secondary progressive MS differ in fundamental ways. PPMS starts with steady progression from the beginning. SPMS develops after years of relapsing remitting disease.
Both types involve gradual worsening and accumulating disability. The symptoms overlap significantly between the two. But the disease history clearly separates them.
Understanding your specific MS type helps you plan better. It guides treatment decisions and sets realistic expectations. Work closely with your healthcare team to monitor your disease.
Treatment options continue improving for both progressive types. Research advances bring new hope regularly. Stay informed about emerging therapies.
Frequently Asked Questions
Is Primary Progressive MS worse than Secondary Progressive MS?
Neither type is inherently worse than the other. Both involve gradual worsening and disability accumulation. Progression rate varies significantly among individuals in both types. Some people with PPMS progress slowly while some with SPMS progress faster. Individual factors like age, lesion location, and treatment response matter more than MS type alone.
How common is PPMS compared to SPMS?
PPMS is much less common than SPMS. Only 10 to 15 % of people have PPMS at diagnosis. About 50 % of people with RRMS eventually develop SPMS. This makes SPMS more prevalent overall since most people start with RRMS.
Does PPMS progress faster than SPMS?
Progression rates vary widely in both types. Some research suggests similar progression rates once steady worsening begins. PPMS might seem faster because it starts with progression. SPMS has years of RRMS before progression starts. Individual progression depends on many factors beyond just MS type.
Are MRI results different in PPMS and SPMS?
Yes, MRI patterns often differ between types. PPMS typically shows more spinal cord involvement and fewer brain lesions. SPMS usually has more brain lesions accumulated from years of RRMS. Both types show gradual lesion accumulation over time. The pattern of new lesions might be less dramatic in PPMS.